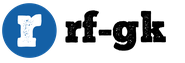Types of placentation in multiple pregnancies. Multiple pregnancy: management, complications, childbirth. Features of the course of multiple pregnancy
 Do you want to know when you should finally meet your long-awaited baby ?! This calculator will help you calculate the expected due date as accurately as possible, as well as tell you when the pregnancy will be considered full-term, and what additional examinations you will have to undergo if you suddenly step over the 41st week of pregnancy.
Do you want to know when you should finally meet your long-awaited baby ?! This calculator will help you calculate the expected due date as accurately as possible, as well as tell you when the pregnancy will be considered full-term, and what additional examinations you will have to undergo if you suddenly step over the 41st week of pregnancy. TESTS DURING PREGNANCY
A complete list of all tests (mandatory and optional), screening (prenatal) tests and ultrasound examinations (US), which are prescribed to pregnant women. Find out what each analysis and examination is for, at what stages of pregnancy they need to be taken, how to decipher the test results (and what are the standards for these indicators), which tests are mandatory for all women, and which are prescribed only if there are indications.PREGNANCY CALCULATOR
The pregnancy calculator, based on the date of your last menstrual period, will calculate your fertile days (those on which it is possible to conceive a child), tell you when it’s time to take a home pregnancy test, when the baby’s first organs begin to develop, when it’s time to visit an antenatal clinic, when to get tested (and which ones), when you feel the first movements of your baby, when you go on “maternity” (prenatal) leave, and finally - when you have to give birth!Conceiving, carrying and having several children at the same time is usually considered a miracle and something unusual. However, cases of the birth of two, three, and sometimes more children are becoming more and more frequent. It is important to understand that childbirth in such a situation is more difficult and is fraught with a high risk of developing the wrong course of the process.
Characteristics of multiple pregnancies
Multiple pregnancies are understood as the process of conceiving, as well as carrying several children at once.
Cases of pregnancy with two or three children are more common, but conception and more fetuses are rare.
There are 2 options for fertilizing eggs for conceiving twins:
- Monochorionic twins or identical twins.
- Bichorial twins or fraternal twins.
 In the first case, one mother's egg is fertilized simultaneously by several of the father's sperm.
In the first case, one mother's egg is fertilized simultaneously by several of the father's sperm.
Thus, children develop in the same amniotic fluid. They are surrounded by shared amniotic fluid.
Identical twins are born of the same sex and very similar (almost identical).
Bichorionic biamniotic twins are a variant of multiple pregnancies, when the mother's body produces several eggs at once.
Children develop in separate amniotic sacs. Amniotic fluid is also different. People born in this type of development are not similar in appearance, and can also be heterosexual.
For a person, the birth of several children is rare.
In the case of eco, the likelihood of having twins increases dramatically. This is due to the fact that several fertilized eggs are placed in the uterus. Necessary to increase the likelihood of successful engraftment.
All eggs, which have already begun the process of their division, are safely fixed at once.
A woman becomes the proud owner of a multiple pregnancy.
Factors affecting the occurrence of multiple pregnancies
 Causes ,
which to a large extent provoke the conception of several children at once and the development of multiple pregnancies:
Causes ,
which to a large extent provoke the conception of several children at once and the development of multiple pregnancies:
- Mother's age;
- Racial affiliation. The likelihood of conceiving twins is greatest among African peoples;
- Genetic predisposition;
- The most favorable season for conceiving twins is spring;
- A short menstrual cycle that does not exceed 21 days;
- Pathological structure of the uterus;
Statistics have established that at the time of cataclysms and wars, the likelihood of several children being born at once increases significantly.
Diagnosis of multiple pregnancies
 In order to accurately determine the presence of several embryos and, as a result, multiple pregnancies, it is imperative to undergo examinations:
In order to accurately determine the presence of several embryos and, as a result, multiple pregnancies, it is imperative to undergo examinations:
- Examination on a gynecological chair.
When going through these procedures, signs of multiple pregnancy are noted:
- A rapid increase in the size of the uterus;
- Inconsistency of the size of the uterus with the expected gestational age;
- The girth of the abdomen is higher than normal for a certain period;
- Low location of the uterus together with the high standing of its bottom;
- During the ultrasound procedure, several fetal eggs are diagnosed.
 A woman may notice the first signs of multiple pregnancy in her early stages:
A woman may notice the first signs of multiple pregnancy in her early stages:
- Increased feeling of tiredness;
- in the morning hours;
- Early sensations of movement;
- The blood level is higher than normal;
- A sharp increase in body weight;
- Fast .
For how long the presence of twins in the uterine cavity will be determined depends entirely on the woman.
The sooner she goes to the antenatal clinic, the sooner the presence of multiple pregnancies will be established.
Features of multiple pregnancy
 On the one hand, multiple pregnancies are no different from the process of carrying one child. But on the other hand, the load on the woman's body is much higher.
On the one hand, multiple pregnancies are no different from the process of carrying one child. But on the other hand, the load on the woman's body is much higher.
This, in turn, can provoke development, as well as a number of features of the course of this process.
In women carrying several children, the following manifestations can be observed:
- Severe shortness of breath;
- Increased fatigue;
- Difficulty functioning of the lungs, lack of oxygen;
- Frequent urination;
- Constipation.
 These negative manifestations are provoked by the rapid growth of the uterus, due to which the diaphragm shifts sharply and the pressure on the pelvic area increases.
These negative manifestations are provoked by the rapid growth of the uterus, due to which the diaphragm shifts sharply and the pressure on the pelvic area increases.
Against the background of these changes in women, it is also noted:
- Toxicosis;
- Development of polyhydramnios in one fetus with simultaneous oligohydramnios in another;
- or late toxicosis;
- arterial pressure;
- Increased swelling;
- Reduced hemoglobin content in the blood and, as a result,.
 Labor often occurs with multiple pregnancies. However, even at birth at term, children are usually born small, but this does not affect their development.
Labor often occurs with multiple pregnancies. However, even at birth at term, children are usually born small, but this does not affect their development.
Multiple pregnancies require special supervision by doctors.
In medical practice, situations are often encountered when one child does not receive the necessary substances. This can provoke congenital malformations.
The position of the fetus in the uterus with twins
Most often, children with the development of multiple pregnancies are located longitudinally relative to each other.
The following variations can be observed:
- Both children are in cephalic presentation;
- Both babies breech;
- One child in cephalic presentation, the second in breech presentation.
During childbirth, babies can change their position. This applies to the child who is born second.
Due to the appearance of additional space after the birth of the first baby, he may turn to a different position.
There may be cases of the pathological situation of children.
This includes lateral and oblique arrangement. However, such options are extremely rare.
The course of labor with multiple pregnancies
 For women who carry several babies, the premature onset of the labor process is characteristic. This phenomenon is considered normal and physiological.
For women who carry several babies, the premature onset of the labor process is characteristic. This phenomenon is considered normal and physiological.
According to statistics, the timing of childbirth in multiple pregnancies is 2-3 weeks earlier.
The course of natural childbirth in this type of pregnancy is accompanied by:
- high risks of occurrence and a wide variety of complications for a woman's health;
- high probability of death of children;
- pathologies of children's health;
- difficult postpartum recovery period.
Natural delivery in the presence of several children at once is fraught with the development of serious complications.
Modern obstetric practice considers multiple pregnancies to be a mandatory indication for surgery.
Complications during childbirth and in the postpartum period
 The very presence of such a pregnancy for a person is abnormal, therefore, childbirth is very often accompanied by a number of complications:
The very presence of such a pregnancy for a person is abnormal, therefore, childbirth is very often accompanied by a number of complications:
- Simultaneous entry into the pelvis of the heads of children;
- Collision of twins;
- Intrauterine death of one of the children due to lack of nutrition or developmental defects;
- Multiple developmental defects in one of the children;
- Fusion of children among themselves.
Usually, these complications are fatal for both the mother and future children. Therefore, in the early stages, it is recommended to terminate such a pregnancy.
Even with the birth of healthy children, the postpartum period for a woman is also likely to be accompanied by complications:
- Bleeding in the uterus;
- Incomplete removal of the placenta;
- Poor contractility of the uterus;
- Overstretching of the uterus;
- Decreased tone of the uterus;
- Infectious diseases of the female reproductive system.
Labor management
 For the correct management of the generic process, it is necessary to determine the following indicators:
For the correct management of the generic process, it is necessary to determine the following indicators:
- Pregnancy period in weeks;
- Presentation and arrangement of children;
- Estimated weight of children;
- Amniotic fluid amount;
- The number of amniotic sacs;
Only after collecting a complete history can you choose the right delivery method, which will reduce the risks of complications to a minimum.
 Indications for natural delivery:
Indications for natural delivery:
- Cephalic presentation of a baby who should be born first;
- The integrity of the amniotic fluid;
- Good labor activity;
- Absence of pathological conditions in children;
- High dynamics of neck opening.
However, childbirth in the presence of twins is carried out by caesarean section. This is due to the fact that even in the absence of complications, the birth of several children is too risky for health.
Natural childbirth in women expecting twins, and even more so triplets, is now practically excluded.
Indications for cesarean section in multiple pregnancies
 The following reasons may become a mandatory indication for delivery through a cesarean section:
The following reasons may become a mandatory indication for delivery through a cesarean section:
- The pelvic location of one of the children;
- The woman is over 30 years old;
- The presence of scars on the uterus;
- Complications during natural childbirth.
On the one hand, multiple pregnancy is a magical event for expectant parents, on the other hand, it is fraught with many dangers and complications.
It is very important to diagnose this type of pregnancy as early as possible and is constantly under the regular supervision of doctors.
This will minimize the risks of pathologies and complications, give birth to healthy children.
Video: childbirth with multiple pregnancies
Thank you
The site provides background information for informational purposes only. Diagnosis and treatment of diseases must be carried out under the supervision of a specialist. All drugs have contraindications. A specialist consultation is required!
Multiple pregnancy - definition and varieties (twins and twins)
Multiple pregnancy- this is a pregnancy in which not one, but several (two, three or more) fetuses develop in the woman's uterus at the same time. Usually the name of multiple pregnancy is given depending on the number of fetuses: for example, if there are two children, then they talk about pregnancy with twins, if three, then triplets, etc.Currently, the frequency of multiple pregnancies ranges from 0.7 to 1.5% in various countries in Europe and the United States. The widespread and relatively frequent use of assisted reproductive technologies (IVF) has led to an increase in the incidence of multiple pregnancies.
Depending on the mechanism of the appearance of twins, there are dizygotic (double) and monozygous (identical) multiple pregnancies. Children of fraternal twins are called twins, and children of identical twins are called twins or twins. Among all multiple pregnancies, the frequency of twin twins is about 70%. Twins are always of the same sex and are like two drops of water similar to each other, since they develop from one fetal egg and have exactly the same set of genes. Twins can be of different sexes and are similar only as siblings, since they develop from different eggs, and, therefore, have a different set of genes.
A twin pregnancy develops as a result of the fertilization of two eggs at the same time, which are implanted in different parts of the uterus. Quite often, the formation of fraternal twins occurs as a result of two different sexual acts, carried out with a small interval between each other - no more than a week. However, fraternal twins can also be conceived during one sexual intercourse, provided that there is a simultaneous maturation and release of two eggs from the same or different ovaries. With twin twins, each fetus necessarily has its own placenta and its own fetal bladder. The position of the fetus, when each of them has its own placenta and fetal bladder, is called bichorionic biamniotic twins. That is, in the uterus there are simultaneously two placentas (bichorial twins) and two fetal bladders (biamniotic twins), in each of which the child grows and develops.
Identical twins develop from one ovum, which, after fertilization, divides into two cells, each of which gives rise to a separate organism. With identical twins, the number of placentas and fetal bladders depends on the time of separation of a single fertilized egg. If separation occurs within the first three days after fertilization, while the ovum is in the fallopian tube and has not attached to the wall of the uterus, then two placentas and two separate fetal sacs will form. In this case, there will be two fetuses in the uterus in two separate fetal bladders, each feeding from its placenta. Such twins are called bichorial (two placentas) biamniotic (two fetal bladders).
If the ovum divides on 3 - 8 days after fertilization, that is, at the stage of attachment to the uterine wall, then two fetuses are formed, two fetal bladders, but one placenta for two. In this case, each twin will be in its own fetal bladder, but they will feed from one placenta, from which two umbilical cords will depart. This version of twins is called monochorionic (one placenta) biamniotic (two fetal bladders).
If the ovum divides between 8 and 13 days after fertilization, then two fetuses will form, but one placenta and one fetal bladder. In this case, both fetuses will be in one for two fetal bladder, and feed from the same placenta. Such twins are called monochorionic (one placenta) monoamniotic (one fetal bladder).
If the fertilized egg divides later than 13 days after fertilization, then Siamese twins develop as a result, which are fused with different parts of the body.
From the point of view of safety and normal development of the fetus, the best option is bichorionic biamniotic twins, both identical and fraternal. Monochorionic biamniotic twins develop worse and the risk of pregnancy complications is higher. And the most unfavorable variant of twins are monochorionic monoamniotic ones.
The likelihood of multiple pregnancies
The probability of multiple pregnancy with absolutely natural conception is no more than 1.5 - 2%. Moreover, in 99% of multiple pregnancies are represented by twins, and triplets and a large number of fetuses in only 1% of cases. With natural conception, the likelihood of multiple pregnancy increases in women over 35 years old or at any age in the spring season against the background of a significant lengthening of daylight hours. In addition, in women in whose family twins or twins have already been born, the likelihood of multiple pregnancy is higher than that of other representatives of the fairer sex.However, if pregnancy occurs under the influence of drugs or assisted reproductive technologies, then the likelihood of twins or triplets is significantly higher than with natural conception. So, when using drugs to stimulate ovulation (for example, Clomiphene, Clostilbegit, etc.), the likelihood of multiple pregnancy increases to 6 - 8%. If, to improve the chances of conception, drugs containing gonadotropin were used, then the probability of twins is already 25 - 35%. If a woman becomes pregnant with the help of assisted reproductive technologies (IVF), then the probability of multiple pregnancy in such a situation is 35 to 40%.
Multiple pregnancy with IVF
 If a woman becomes pregnant using IVF (in vitro fertilization), then the probability of multiple pregnancy is, according to various researchers, from 35% to 55%. In this case, a woman may have twins, triplets or fours. The mechanism of multiple pregnancy with IVF is very simple - four embryos are simultaneously implanted into the uterus, hoping that at least one of them will take root. However, not one, but two, three or all four embryos can take root, that is, implanted into the wall of the uterus, as a result of which a woman develops a multiple pregnancy.
If a woman becomes pregnant using IVF (in vitro fertilization), then the probability of multiple pregnancy is, according to various researchers, from 35% to 55%. In this case, a woman may have twins, triplets or fours. The mechanism of multiple pregnancy with IVF is very simple - four embryos are simultaneously implanted into the uterus, hoping that at least one of them will take root. However, not one, but two, three or all four embryos can take root, that is, implanted into the wall of the uterus, as a result of which a woman develops a multiple pregnancy. If during the ultrasound after IVF a multiple pregnancy (triplets or quadruplets) was detected, then the woman is offered to "remove" the extra embryos, leaving only one or two. If twins are found, then the embryos are not offered to be removed. In this case, the decision is made by the woman herself. If she decides to keep all three or four embryos that have taken root, then she will have a quadruple or triplets. The further development of multiple pregnancies that developed as a result of IVF is no different from the natural one.
Reduction in multiple pregnancies
Removal of the "extra" embryo in multiple pregnancies is called reduction. This procedure is offered to women who have more than two fetuses in the uterus. Moreover, at present, the reduction is offered not only to women who become pregnant with triplets or quadruples as a result of IVF, but also naturally conceived more than two fetuses at the same time. The aim of the reduction is to reduce the risk of obstetric and perinatal complications associated with multiple pregnancies. During reduction, two fetuses are usually left, since there is a risk of spontaneous death of one of them in the future.The reduction procedure for multiple pregnancies is carried out only with the consent of the woman and on the recommendation of a gynecologist. In this case, the woman herself decides how many fruits to reduce, and how much to leave. Reduction is not carried out against the background of the threat of termination of pregnancy and in acute inflammatory diseases of any organs and systems, since against such an unfavorable background, the procedure can lead to the loss of all fetuses. The reduction can be carried out up to 10 weeks of pregnancy. If you do this at a later stage of pregnancy, then the remnants of fetal tissue will irritate the uterus and provoke complications.
Currently, reduction is performed by the following methods:
- Transcervical. A flexible and soft catheter connected to a vacuum aspirator is inserted into the cervical canal. Under ultrasound guidance, the catheter is advanced to the embryo to be reduced. After the tip of the catheter reaches the fetal membranes of the reduced embryo, a vacuum aspirator is turned on, which tears it off the uterine wall and sucks it into the container. Basically, transcervical reduction is essentially an incomplete vacuum abortion, during which not all fetuses are removed. The method is quite traumatic, therefore it is rarely used now;
- Transvaginal. It is performed under anesthesia in the operating room similar to the process of oocyte collection for IVF. The biopsy adapter is inserted into the vagina and, under ultrasound control, the embryo to be reduced is punctured with a puncture needle. Then the needle is removed. This method is currently the most commonly used;
- Transabdominal. It is performed in the operating room under general anesthesia similar to the procedure for amniocentesis. A puncture is made on the abdominal wall, through which a needle is inserted into the uterus under ultrasound control. The embryo to be reduced is pierced with this needle, after which the instrument is removed.
The most prolific pregnancy
 At present, the most multiple recorded and confirmed pregnancy was the decay, when ten fetuses were simultaneously in the woman's uterus. As a result of this pregnancy, a resident of Brazil in 1946 gave birth to two boys and eight girls. But, unfortunately, all the children died before reaching the age of six months. There are also references to the birth of the tithe in 1924 in Spain and in 1936 in China.
At present, the most multiple recorded and confirmed pregnancy was the decay, when ten fetuses were simultaneously in the woman's uterus. As a result of this pregnancy, a resident of Brazil in 1946 gave birth to two boys and eight girls. But, unfortunately, all the children died before reaching the age of six months. There are also references to the birth of the tithe in 1924 in Spain and in 1936 in China. To date, the most multiple pregnancy that can successfully result in the birth of healthy children without deviations is the gear. If there are more than six fetuses, then some of them suffer from developmental delay, which persists throughout their life.
Multiple pregnancy - delivery time
As a rule, multiple pregnancies, regardless of the method of its development (IVF or natural conception), ends earlier than the term of 40 weeks, since the woman begins premature birth due to excessively strong stretching of the uterus. As a result, babies are born prematurely. Moreover, the greater the number of fetuses, the earlier and more often preterm labor develops. With twins, as a rule, childbirth begins at 36 - 37 weeks, with triplets - at 33 - 34 weeks, and with a quadruple - at 31 weeks.Multiple pregnancy - causes
 Currently, the following possible causal factors have been identified that can lead to multiple pregnancy in a woman:
Currently, the following possible causal factors have been identified that can lead to multiple pregnancy in a woman: - Genetic predisposition. It has been proven that women whose grandmothers or mothers gave birth to twins or twins are 6 to 8 times more likely to have multiple pregnancies than other women. Moreover, most often multiple pregnancies are transmitted through a generation, that is, from grandmother to granddaughter;
- The age of the woman. In women over 35, under the influence of hormonal premenopausal changes in each menstrual cycle, not one, but several eggs can ripen, so the likelihood of multiple pregnancies in adulthood is higher than in young or young. The likelihood of multiple pregnancies is especially high in women over 35 who have given birth before;
- The effects of drugs. Any hormonal agents used to treat infertility, stimulate ovulation or menstrual irregularities (for example, oral contraceptives, Clomiphene, etc.) can lead to the maturation of several eggs at the same time in one cycle, resulting in multiple pregnancies;
- A large number of births in the past. It has been proven that multiple pregnancies mainly develop in re-pregnant women, and its likelihood is the higher, the more births a woman has in the past;
- In Vitro Fertilization. In this case, several eggs are taken from a woman, fertilized with male sperm in a test tube, and the resulting embryos are implanted into the uterus. In this case, four embryos are immediately introduced into the uterus so that at least one can implant and begin to develop. However, two, three, and all four implanted embryos can take root in the uterus, as a result of which a multiple pregnancy develops. In practice, twins are most common as a result of IVF, and triplets or quadruplets are rare.
Signs of multiple pregnancy
Currently, the most informative method for diagnosing multiple pregnancies is ultrasound, but the clinical signs on which doctors of the past were based still play a role. These clinical signs of multiple pregnancy allow a doctor or a woman to suspect the presence of several fetuses in the uterus and, on the basis of this, make a targeted ultrasound examination, which will confirm or refute the assumption with 100% accuracy.So, the signs of multiple pregnancy are the following data:
- Too large size of the uterus, not corresponding to the date;
- Low position of the head or pelvis of the fetus above the entrance to the pelvis in combination with the high standing of the fundus of the uterus, which does not correspond to the date;
- Discrepancy between the size of the fetal head and the volume of the abdomen;
- Large belly volume;
- Excessive weight gain;
- Listening to two heartbeats;
- The concentration of hCG and lactogen is twice the norm;
- Fatigue of a pregnant woman;
- Early and severe toxicosis or gestosis;
- Obstinate constipation;
- Severe swelling of the legs;
- High blood pressure.
How to identify multiple pregnancies - effective diagnostic methods
Currently, multiple pregnancies are detected with 100% accuracy during conventional ultrasound. Also, the determination of the concentration of hCG in the venous blood has a relatively high accuracy, however, this laboratory method is inferior to ultrasound. That is why ultrasound is the method of choice for diagnosing multiple pregnancies.Ultrasound diagnostics of multiple pregnancy
 Ultrasound diagnostics of multiple pregnancies is possible in the early stages of gestation - from 4 to 5 weeks, that is, literally immediately after a delay in menstruation. During an ultrasound scan, the doctor sees several embryos in the uterine cavity, which is undoubted evidence of multiple pregnancy.
Ultrasound diagnostics of multiple pregnancies is possible in the early stages of gestation - from 4 to 5 weeks, that is, literally immediately after a delay in menstruation. During an ultrasound scan, the doctor sees several embryos in the uterine cavity, which is undoubted evidence of multiple pregnancy. The number of placentas (chorionicity) and fetal bladders (amnioticity), and not the dichotomy or mono-ovulation of the fetus, is of decisive importance for the choice of tactics for managing pregnancy and calculating the risk of complications. The most favorable course of pregnancy is with bichorionic biamniotic twins, when each fetus has its own placenta and fetal bladder. The least favorable and with the maximum possible number of complications is monochorionic monoamniotic pregnancy, when two fetuses are in the same fetal bladder and are fed from the same placenta. Therefore, during an ultrasound scan, the doctor counts not only the number of fetuses, but also determines how many placentas and fetal blisters they have.
In multiple pregnancies, ultrasound plays a huge role in identifying various defects or fetal growth retardation, since biochemical screening tests (determining the concentration of hCG, AFP, etc.) are not informative. Therefore, the identification of malformations by ultrasound in multiple pregnancies must be performed in the early stages of gestation (from 10 to 12 weeks), while assessing the condition of each fetus separately.
HCG in the diagnosis of multiple pregnancies
HCG in the diagnosis of multiple pregnancies is a relatively informative method, but inaccurate. The diagnosis of multiple pregnancies is based on the excess of the hCG level of normal concentrations for each specific gestational age. This means that if the concentration of hCG in a woman's blood is higher than normal for a given gestational age, then she has not one, but several fetuses. That is, with the help of hCG, it is possible to identify multiple pregnancies, but it is impossible to understand how many fetuses are in the woman's uterus, in one fetal bladder or in different ones, they have two placentas or one is impossible.The development of multiple pregnancies
 The process of developing multiple pregnancies creates a very high load on the mother's body, since the cardiovascular, respiratory, urinary systems, as well as the liver, spleen, bone marrow and other organs continuously work in an enhanced mode for a rather long period of time (40 weeks) to ensure that one, but two or more growing organisms are all necessary. Therefore, the incidence in women carrying multiple pregnancies is 3 to 7 times higher than in singleton pregnancies. Moreover, the more fetuses in a woman's uterus, the higher the risk of complications from various organs and systems of the mother.
The process of developing multiple pregnancies creates a very high load on the mother's body, since the cardiovascular, respiratory, urinary systems, as well as the liver, spleen, bone marrow and other organs continuously work in an enhanced mode for a rather long period of time (40 weeks) to ensure that one, but two or more growing organisms are all necessary. Therefore, the incidence in women carrying multiple pregnancies is 3 to 7 times higher than in singleton pregnancies. Moreover, the more fetuses in a woman's uterus, the higher the risk of complications from various organs and systems of the mother. If a woman, before the onset of multiple pregnancy, suffered from any chronic diseases, then they will necessarily become aggravated, since the body is under very strong stress. In addition, with multiple pregnancies, half of women develop preeclampsia. All pregnant women in the second and third trimesters develop edema and arterial hypertension, which are a normal reaction of the body to the needs of the fetus. A fairly standard complication of multiple pregnancies is anemia, which must be prevented by taking iron supplements throughout the entire period of bearing children.
For the normal growth and development of several fetuses, a pregnant woman must eat well and vigorously, since her need for vitamins, trace elements, proteins, fats and carbohydrates is very high. The daily calorie intake of a woman carrying twins should be at least 4500 kcal. Moreover, these calories should be recruited from nutrient-rich foods, and not chocolate and flour products. If a woman with multiple pregnancies eats poorly, then this leads to the depletion of her body, the development of severe chronic pathologies and numerous complications. During a multiple pregnancy, a woman normally gains 20 - 22 kg in weight, with 10 kg in the first half.
In multiple pregnancies, one fetus is usually larger than the second. If the difference in body weight and height between fruits does not exceed 20%, then this is considered the norm. But when the weight and growth of one fetus exceeds the second by more than 20%, they speak of a delay in the development of the second, too small child. A delay in the development of one of the fetuses in multiple pregnancies is noted 10 times more often than in single pregnancies. Moreover, the likelihood of developmental delay is highest in monochorionic pregnancy and minimal in bichorionic biamniotic pregnancy.
Multiple pregnancies usually end prematurely because the uterus is stretching too much. With twins, childbirth usually occurs at 36 - 37 weeks, with triplets, at 33 - 34 weeks, and with a quadruple, at 31 weeks. Due to the development of several fetuses in the uterus, they are born with a smaller weight and body length compared to those born from a singleton pregnancy. In all other aspects, the development of multiple pregnancies is exactly the same as that of singleton pregnancies.
Multiple pregnancy - complications
With multiple pregnancies, the following complications can develop:- Early pregnancy miscarriage;
- Premature birth;
- Intrauterine death of one or both fetuses;
- Severe gestosis;
- Bleeding in the postpartum period;
- Hypoxia of one or both fetuses;
- Fetal collision (clutching of two fruits by their heads, as a result of which they simultaneously end up at the entrance to the small pelvis);
- Syndrome of fetofetal blood transfusion (SFFG);
- Reverse arterial perfusion;
- Congenital malformations of one of the fetuses;
- Delayed development of one of the fetuses;
- Fusion of fruits with the formation of Siamese twins.
Another specific complication of multiple pregnancies is fetal fusion. Such accreted children are called Siamese twins. Fusion is formed in those parts of the body with which the fruits are most in contact. Most often, fusion occurs with the chest (thoracopagi), abdomen in the navel (omphalopagi), skull bones (craniopagi), coccyx (pygopagi) or sacrum (ischiopagi).
In addition to the above, with multiple pregnancies, exactly the same complications can develop as with a singleton.
Childbirth with multiple pregnancies
If the multiple pregnancy proceeded normally, the fetuses have a longitudinal arrangement, then delivery is possible in a natural way. With multiple pregnancies, complications during childbirth develop more often than with single pregnancies, which leads to a higher frequency of emergency caesarean sections. A woman with multiple pregnancies should be hospitalized in a maternity hospital 3-4 weeks before the expected date of birth, and not wait for the onset of labor at home. The stay in the maternity hospital is necessary for examination and assessment of the obstetric situation, on the basis of which the doctor will decide on the possibility of natural childbirth or on the need for a planned caesarean section.The generally accepted tactic of delivery in multiple pregnancies is as follows:
1.
If the pregnancy proceeded with complications, one of the fetuses is in a transverse position or both are in breech presentation, the woman has a scar on the uterus, then a planned cesarean section is performed.
2.
If a woman approached childbirth in a satisfactory condition, the fetuses are in a longitudinal position, then it is recommended to carry out childbirth through natural routes. With the development of complications, an emergency cesarean section is performed.
Currently, with multiple pregnancies, as a rule, a planned cesarean section is performed.
Multiple pregnancy: causes, varieties, diagnosis, childbirth - video
When they give sick leave (maternity leave) with multiple births
pregnancy
 With multiple pregnancies, a woman will be able to receive a sick leave (maternity leave) two weeks earlier than with a singleton, that is, within 28 weeks. All other rules for issuing sick leave and cash benefits are exactly the same as for singleton pregnancies.
With multiple pregnancies, a woman will be able to receive a sick leave (maternity leave) two weeks earlier than with a singleton, that is, within 28 weeks. All other rules for issuing sick leave and cash benefits are exactly the same as for singleton pregnancies. Multiple pregnancy- This is a pregnancy in which two or more fetuses develop in a woman's body.
Information The widespread use of reproductive methods at the moment has led to a significant increase in multiple pregnancies (up to 2% of all pregnancies).
Causes of multiple pregnancies
The main factors that increase the possibility of multiple pregnancies:
- Pelvic or transverse presentation of at least one of the fetuses;
- Monochorionic monoamniotic twins;
- Conjoined twins;
- Overstretching of the uterus due to the large size of the fetus or pronounced polyhydramnios.
Moreover, indications for operative delivery may arise urgently at the beginning of the birth management through the vaginal birth canal:
- Weakness of labor;
- Premature detachment of a normally located placenta;
- Acute hypoxia or asphyxia of one or both fetuses;
- Loops of the umbilical cord or small parts of the fetus.
Despite the relatively high modern level of development of obstetrics and obstetrics, women with multiple births are still at high risk. The management of multiple pregnancies and childbirth itself are significantly different from the usual pregnancy with one fetus. They require experience and in-depth knowledge of this condition from medical personnel.
Relevance of the topic
Features of multiple pregnancies determine the relevance of the problem for obstetrics in general and, in particular, for obstetrics of the perinatal period (from 22 weeks of intrauterine development to 28 weeks of the postpartum period). These features are a high percentage of complications, prematurity and the risk of premature birth, severe placental insufficiency, fetal malnutrition and intrauterine hypoxia, the possibility of severe malformations, etc.
Perinatal mortality in multiple pregnancies, compared with singleton pregnancies, is about 10% and is largely related to fetal body weight. Malformations are recorded 2 times more often, intrauterine mortality is 3-4 times higher, and over the past 30 years it has practically not decreased. The incidence of cerebral palsy in a child of twins is 3-7 times more often, triplets - 10 times, and the number of complications in the mother throughout the entire period of pregnancy - 2 or more times (up to 10).
Causes of multiple pregnancies
The development of two or more fetuses in a woman's body is called multiple pregnancy. Over the past 20 years, it has doubled, and women with multiple pregnancies accounted for 0.7-1.5% of all pregnant women, the birth of twins in relation to the number of all births - 1: 87, triplets - 1: 6 400, fours - 1: 51,000.
Many reasons for multiple pregnancy have been noted, which indicates that this issue is still insufficiently studied. The likelihood of multiple pregnancies is largely determined by the following factors:
- Heredity, that is, if the spouses or one of them come from multiple pregnancies or in their families, especially in the female line, there have been similar cases.
- An increased content of follicle-stimulating hormone in a woman's blood, which promotes the development and maturation of two or more eggs at the same time. This may be due to heredity, the use of drugs that stimulate ovulation in the treatment of infertility, pregnancy immediately after the abolition of ok (), especially against the background of the use of ovulatory stimulation agents.
- In vitro fertilization (), the program of which includes drug hyperstimulation of the ovaries to obtain a large number of mature eggs. Multiple pregnancy with IVF is also due to the implantation of several fertilized eggs into the uterine cavity, the possibility of implantation and development of more than one.
- The number of births: with repeated pregnancies and childbirth, the likelihood of multiple births increases.
- The woman is over 35 years old. This is thought to be due to a decrease in fertility at this age due to the lack of monthly ovulation. As a result, there is an accumulation of hormones and their effect in the form of ovulation of two or more eggs.
- Anomalies in the development of internal genital organs.
The many causes of multiple pregnancies, the main ones of which are listed above, indicate that this issue is still insufficiently understood.
Classification of multiple pregnancies

In deciding the tactics of managing such a pregnancy and childbirth, zygosity, chorionicity and the number of amniotic cavities are of considerable importance. A zygote is a cell formed from the fusion of an egg with a sperm and contains a complete double set of chromosomes. Chorion is one of the three (outer) membranes of the fetus. The amniotic cavity is a cavity bounded by an aqueous membrane (amnion) and filled with amniotic fluid.
Monozygous
In accordance with the number of fetuses, pregnancy is distinguished by twins, triplets, etc. About 30% of twins are formed from one fertilized egg. Subsequently, as a result of its division, two similar structures develop, which have the ability to develop independently, individually. This type of twins is called monozygous, or identical, and children are called twins. They have the same sex, eye and hair color, skin pattern of fingers, blood type, position and shape of teeth.
Bizygotic
The simultaneous maturation and release of two or more eggs can occur both in one ovary and in both during one menstrual cycle. Bizygotic, or bilingual embryos develop from two fertilized eggs and make up an average of 70%. Children are called "twins." They can be either same-sex or heterosexual, with the same or different blood groups and be in the same genetic relationship. In cases of a larger number (triplets, quadruplets, etc.), both monozygosity and dysygosity in various combinations are possible.
Each of the double embryos has its own chorial / placental and amniotic membranes. Each embryo has its own placenta. Thus, a four-layer septum is formed between the two embryos, consisting of sections of two chorionic / placental and two amniotic membranes. Therefore, such embryos in the classification are called di- (or bi-) - chorial, diamniotic dizygotic twins.
The formation of identical twins occurs at the early stages of development, division and transformation of a fertilized egg and depends on the time of these processes:
- If the division of the egg occurs within the first 72 hours, counting from the moment of fertilization, that is, before the formation of the inner cell layer and the change in the cells of the outer layer of the egg, then two chorions and two amniotic cavities develop. As a result, dichorial, diamniotic monozygous twins are formed, in which one placenta is possible, formed from the fusion of two placentas, or two separate placentas.
- If the oocyte division occurs within 4-8 days after fertilization, when the formation of the inner cell layer has already ended, and the chorion has begun to form from the outer layer, but the amniotic membranes are not yet laid, then each embryo will develop in a separate amniotic cavity. Thus, embryos with individual water sacs will be surrounded by one common chorion, as a result of which diamniotic, monochorionic monozygous twins develop.
- If the laying of the amniotic membrane has already taken place at the time of separation of the ovum, which usually occurs by the 8th day after the fusion of the egg with the sperm, this will lead to the development of embryos with a common water sac and one chorion - monoamniotic, monochorionic monozygous twins.
- The division of a fertilized egg at a later date (after 13 days), when the embryonic disc has already formed, will be only partial. This will lead to the development of twins who have grown together.
The easiest way to determine whether you are identical or fraudulent is to be examined by an obstetrician after the birth of children. The septum between the twins consists of two water (amniotic) membranes, and between the "twins" - of four: two amniotic and two chorionic.
Features of the course of multiple pregnancy

Possible complications for the mother
Pregnancy with two or more fetuses, especially with their different blood groups, in comparison with singleton, makes higher demands on the woman's body. In addition, the flow in the dichorionic type is more severe than in the monochorionic type. The average gestation period for twins is about 37 weeks, for triplets - 35 weeks.
In the body of a pregnant woman, the volume of circulating blood increases (by 50-60%), which creates an additional burden for the cardiac function, while with one fetus this figure does not exceed 40-50%. Due to hemodilution (blood dilution), anemia, an increased need for vitamins, macro- and microelements, especially folic acid and iron, are often noted.
Women are much more likely to note shortness of breath, rapid fatigue, excruciating heartburn, urinary disorders and constipation. They are especially worried about these phenomena in the last stages. In addition, toxicosis and among them are more common, develop earlier, and their course is more severe. The uterus reaches a large size not only because of multiple pregnancies, but also as a result of cases of frequent development of polyhydramnios, which can cause renal dysfunction. The number of premature births is in direct proportion to the number of fetuses and ranges from 25 to 50%.
A very common problem is cervical insufficiency (ICI) in multiple pregnancies. It develops much more often than with singleton, especially in the presence of triplets or more, which is associated with the influence of a mechanical factor (increased pressure in the uterine cavity and its stretching). ICI usually begins to develop after 22 weeks and is characterized by rapid progression. If, with doubles, surgical treatment to strengthen the neck is effective, then as triplets grow, etc., the sutures are often not able to withstand the load and are cut through. Therefore, in some cases, the additional use of a special pessary helps.
With multiple births, chronic somatic diseases also develop more often, exacerbate and become more severe. Multiple pregnancies after cesarean section require special attention and strict constant follow-up, due to the large number of risks for both the fetus and the woman. The main risks with a high frequency include:
- disorders of the placental circulation due to a violation of the vasculature of the uterus after surgery, which leads to intrauterine growth retardation and / or intrauterine asphyxia;
- placenta previa;
- the threat of termination of pregnancy;
- wrong position of the fruit;
- failure of the scar on the uterus and its rupture, which is the most dangerous.
In some cases, in multiple pregnancies, as in singleton pregnancies, on the 8th day, bloody discharge from the vagina is possible, lasting about 4 days - this is, as a rule, minor implantation bleeding that accompanies the introduction (implantation) of a fertilized egg into the mucous membrane uterus. However, when two or more of these eggs are implanted, it can be longer, repeated and abundant and lead to spontaneous miscarriage. In these cases, it is necessary to carry out differential diagnostics and treatment in a hospital setting, where assistance is provided in the form of hemostatic therapy, rest, the appointment of antispasmodics, etc.
Risks to the fetus (s)
Compared with singleton pregnancies, the delay in the development of one fetus in multiple pregnancies occurs 10 times more often and is 20% for dichorionic twins, 30% for monochorionic twins, and the delay in the development of twins as a whole is 1.7% and 7.5%, respectively.
Of fundamental importance in detecting congenital malformations in one of the fetuses is the determination during the prenatal period of zygosity, since in the case of dizygotic twins, the second fetus may be without pathology, and with monozygous twins, the likelihood of defects in one of them is quite high. The likelihood of developing fetal structural anomalies in singleton pregnancies and dizygotic twins is the same, and in the case of monozygous twins, it is 2-3 times higher.
In order to detect trisomy of fetuses, which include Down's disease, Edwards and Patau syndromes, a non-invasive prenatal test is performed with significant reliability. Its essence lies in the genetic study of fetal DNA particles in the venous blood of a woman in the 9th - 24th weeks. In case of a positive result, additional, but already invasive, genetic studies are carried out. When confirming the results, the tactics of further management of pregnancy is to artificially terminate it.

In the monochorionic, much less frequently in the bichorial placenta, there are frequent cases of arterio-arterial or arterio-venous anastomosis (the connection between two arteries or between an artery and a vein). The second type is the most unfavorable, since in this case there is an outflow of blood from the artery of one fetus into the vein of another. In these cases, if the pressure is symmetrical in the system of placental vessels, the development of fetuses occurs under equal conditions. But with monozygous twins, these conditions can be violated with asymmetric blood circulation in the placenta, as a result of which the supply of arterial blood to one of the fetuses decreases, it does not receive sufficient nutrition and its development is delayed.
A significant imbalance in the placental vascular system is the reason that almost all blood circulation goes to one of the twins - the development of fetal-fetal transfusion syndrome (FFTS) is possible, which is noted especially in cases of monochorionic multiple pregnancy (from 5 to 25%), hypertension , heart enlargement, etc. in one of the fruits. The second may develop deformity, cessation of heart function, or he gradually dies and undergoes mummification (spontaneous fetal reduction). This process can be complicated by the development of a woman's DIC syndrome (disseminated intravascular coagulation), which threatens her life.
Fetal reduction in multiple pregnancies
In some cases, the reduction of the fetus is carried out artificially. The need for this is more common after IVF. Artificial reduction is associated with certain risks and complications, and therefore is performed in the presence of strict indications:
- The need to reduce the number of fetuses implanted after IVF.
- Pathological changes in them.
- The risk of miscarriage.
- A woman has contraindications for carrying multiple pregnancies.
The artificial reduction procedure is usually carried out no earlier than 7 and no later than 13 weeks. It consists in stopping the heart of a hopeless fetus (or fetuses) by puncture injection of a special drug or air into his / their heart. To do this, transvaginally (at 7-8 weeks) or transabdominal (at 8-13 weeks) after local anesthesia with a needle under the control of an ultrasound device, a puncture of the uterine cavity is performed. In the future, resorption of fetal tissues occurs.
How to sleep with multiple pregnancies?
Arising in the third trimester in almost half of women with one fetus, the so-called inferior vena cava syndrome, can complicate the course of pregnancy. With multiple pregnancies, it occurs earlier and can be much more severe.
All venous blood is collected in a vein from the lower half of the body and abdominal cavity, then it enters the right atrium, etc. The cause of this syndrome is increased pressure in the abdominal cavity due to the enlargement of the uterus. When a woman is horizontal on her back or on her right side, the inferior vena cava is compressed between the uterus and the spine.
Against the background of an increased volume of circulating blood and a woman's increased need for blood supply to the brain and heart, the supply of the required volume of blood to them when the inferior vena cava is compressed is sharply reduced due to a decrease in the return of arterial blood, and the blood supply to the fetus also suffers. For the majority, this proceeds imperceptibly, but approximately 10% may experience symptoms such as a sharp drop in blood pressure, dizziness, pallor, nausea, vomiting, and in severe cases, loss of consciousness and collapse, and the appearance of seizures are possible.
Blood circulation is quickly restored when the uterus is displaced by the hand to the left or as a result of the woman turning to the left side, which helps to release the inferior vena cava from compression. Therefore, being in a horizontal position, you must lie on your left side.
Signs of multiple pregnancy and its management

Multiple early pregnancy
Diagnostics
Widespread use in clinical practice of obstetrics and gynecology made it possible to diagnose multiple pregnancy in the early stages. Before ultrasound, this diagnosis was often difficult. Basically, it was more or less reliable in the later stages, and sometimes only during childbirth.
How long is multiple pregnancy determined?
An early assumption about the presence of two or more fruits can be made on the basis of a set of signs:
- a history that the married couple or their immediate family members are one of the twins or "twins";
- availability of data on the performed ovulation hyperstimulation and IVF;
- early development and more severe course of induced hypertension, symptoms of toxicosis (vomiting, nausea), swelling of the mammary glands;
- inconsistency in the first trimester of the size of the uterus with the duration of pregnancy, which also occurs with or gallbladder drift.
At a later date, in the formulation of a presumptive diagnosis, importance is attached to such data as:
- early movement during multiple pregnancies, which can be felt by a woman from the 15th week, while with the first singleton - from the 20th, and with subsequent ones - from the 18th week;
- the size of the abdominal circumference and the height of the fundus of the uterus, which exceed the expected timing of a singleton pregnancy;
- palpation through the anterior abdominal wall in the second half of gestation of large ballot pieces of fetuses (heads and pelvis) in different parts of the abdomen;
- palpation of a large number of small parts;
- the presence in the middle sections of the bottom of the uterus of a depression formed by the protrusion of its corners by large fetal parts (with twins);
- auscultatory determination of two points of the heartbeat, especially if there is a zone of absence of tones between them (zone of "silence");
- different (difference in 10 beats) heart rate at different points, which can be determined by means of cardiological monitors.
How to identify multiple pregnancies in the early stages more reliably?
In making such a diagnosis, to a certain extent, one can focus on the concentration of hCG (human chorionic gonadotropin) and placental lactogen in the blood. This laboratory biochemical testing is not entirely reliable, but relatively informative. So, the level of hCG in multiple pregnancies at each stage of the gestational period exceeds the norm for a singleton pregnancy.
Determination of the content of progesterone in the blood is of similar importance. Increased progesterone in multiple pregnancies , in comparison with the norms determined for a singleton, will be in each respective trimester.
The main method of early diagnosis and a means of helping to prevent many complications of multiple pregnancies is ultrasound. The accuracy of this diagnostic method, including the earliest dates, is more than 99%. It is based on the visual identification of several fertilized eggs or embryos from the 5th to the 6th week.
In addition, echography allows in the second and third trimesters to determine the nature of fetal development and the contours of the fetus, which helps to identify fused twins, FFTS, localization and number of placentas and amniotic (water) cavities, to identify congenital malformations, antenatal death, etc. In accordance with echometric biometrics, the following five types of development of twins are distinguished:
- Physiological - both fruits.
- Signs of hypotrophy with uneven (dissociated) development.
- Uneven development of both fetuses with a difference of 10% from the body weight of the largest of them.
- The presence of congenital developmental pathology.
- Intrauterine death of one fetus.

Fetal presentation options
Ultrasound also allows you to establish the presentation of the fetus and their position, which is especially important before the onset of labor.
In addition to some of the above points (reduction, prevention of compression syndrome of the inferior vena cava, etc.), it provides for the prevention of gestosis, their early detection and treatment in a hospital setting, control of the blood coagulation system, the function of the cardiovascular system and renal function.
Recommendations are also given on the correct balanced and sufficiently high-calorie diet for a woman, folic acid intake of 0, 001 grams per day and iron supplements (up to 100 mg) are prescribed. In addition, in order to prevent premature birth, it is recommended to limit physical activity - staying in bed 3 times for 1-2 hours during the day, taking tocolytics and bed rest in case of a threat of premature birth.
One of the ways to predict the resolution of pregnancy is the use of non-stress testing of the state of fetal heart function in response to their movement. The test should be performed every week after the 30-week period. If possible, a blood flow study is also carried out in each of the fetuses separately.
In case of uncomplicated pregnancy, hospitalization in the maternity ward is necessary before the expected due date for 2-3 weeks in the presence of twins and for a month - triplets. In the absence of the onset of labor at a period of 37 weeks, it is advisable to stimulate it, and in some cases - a planned caesarean section at a period of 37-38 weeks. The presence of a scar on the uterus with multiple pregnancies is a direct indication for a cesarean section.
The optimal method of delivery in the case of monochorionic and monoamniotic twins is a caesarean section at 33-34 weeks (due to the high risk of cord torsion), and for pregnancy with 3 or more fetuses - at 34 weeks.
Childbirth and their management

A normal birth course is often accompanied by complications. In the first stage of labor, on average, 30% of women in labor have premature or earlier rupture of amniotic fluid. Moreover, it is often accompanied by the loss of small parts - umbilical cord loops, legs or handles.
Due to the overstretched uterus, weakness of labor forces develops, and the opening of the cervix is significantly delayed. The duration of the period of expulsion of the first fetus often increases. The presenting part of the second tends to be inserted into the pelvis at the same time as the first, and this takes a long time. The muscles of the anterior abdominal wall are weakened and overstretched, due to which the stretching period is lengthened or impossible. All this leads to prolonged labor, which threatens infection of the uterine cavity and the development of hypoxia (oxygen starvation) of the fetus.
During the period of expulsion of premature fetuses, there is a risk of rapid labor and rupture of the perineum. Prevention of this complication requires timely pudendal (perineal) anesthesia and perineal dissection.
A serious complication in the period of expulsion is premature placental abruption, especially after the birth of the first child, which is associated with a sharp decrease in pressure inside the uterus and a decrease in its volume. This complication threatens with profuse bleeding and the development of hypoxia in the second child. To prevent it, the obstetrician performs an emergency opening of the second fetal bladder.
A very rare but difficult complication is the adhesion of the heads to each other, as a result of which they tend to enter the pelvis at the same time.
Labor management in multiple pregnancies
It consists in careful monitoring of the cardiac activity of the fetus with the help of cardiac monitors and the condition of the woman in labor. Their maintenance in the first period is desirable on the left side for the prevention of inferior vena cava syndrome. With the development of the weakness of the labor forces, the latter are stimulated by intravenous drip of a glucose solution with oxytocin, anesthesia with epidural analgesia.
In the case of the development of weakness of labor and fetal hypoxia during the period of expulsion, obstetric surgical aids are carried out in the form of the imposition of obstetric forceps on the head (with cephalic presentation) or extraction (with breech presentation) by the pelvic end.
Ligation of the umbilical cord is carried out not only at the fetal end, but also at the maternal end, since after its dissection with monochorionic twins, the death of the second fetus as a result of bleeding from the umbilical cord is possible.
The birth of the second child should occur no later than 10-15 minutes after the first. Otherwise, the obstetrician opens the fetal bladder, and the amniotic fluid is slowly released, after which childbirth is carried out naturally (with a longitudinal position).
In the case of a transverse position or incorrect insertion of the head of the second fetus into the small pelvis under general anesthesia, the pedicle is rotated and the child is removed. If it is impossible to give birth in a natural way (impossibility of turning, a large child, cervical spasm, signs of acute hypoxia of one of the fetuses, prolapse of the umbilical cord and small parts, persistent secondary birth weakness), delivery is carried out by cesarean section. The optimal delivery option for triplets or more, as well as in the case of twins fusion, is a cesarean section.
The successive period (before the separation of the placenta - the placenta with membranes) proceeds in the same way as in a singleton pregnancy. However, due to the overstretched uterus and a decrease in its tone, the frequency of delayed separation of the placenta and the associated profuse bleeding is much higher and more dangerous. Therefore, at the end of the second period, methylergometrine is administered intravenously, and after the birth of children, oxytocin is injected drip within 2 hours. If there is no effect, manual separation of the placenta and subsequent massage of the uterus on the fist are performed.
The incidence of complications in the postpartum period is also significantly higher. They are manifested by late postpartum bleeding, delayed reverse development of the uterus to the previous state (subinvolution), postpartum. Therefore, after childbirth, anti-inflammatory drugs and uterine-reducing drugs are prescribed.
Thus, despite the fact that multiple pregnancy is not a pathological condition, it requires increased attention and a specific approach to each woman at every stage from conception to the postpartum period. In addition, special supervision and care of the born babies is necessary.